What the Coordination Layer Actually Needs to Look Like
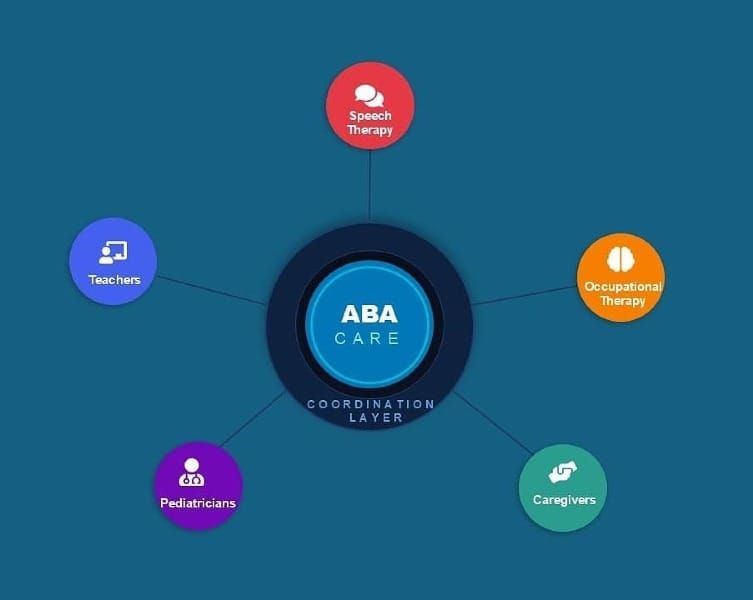
Autism care is often anchored in ABA, typically delivered within a single system. But the care around it is not.
No single system owns coordination. No model fully supports it.
This piece does not attempt to solve that problem. It focuses on something narrower:
what a coordination layer would need to do in practice to make the space between systems usable.
Not as a platform.
Not as an integration.
As a function.
Start with what’s actually missing
It’s tempting to frame the coordination problem as a data problem. The data exists. ABA providers generate detailed session notes, progress reports, goal tracking. Schools produce IEP documentation. Therapists track developmental milestones.
The problem isn’t volume.
It’s that none of it travels.
Each system produces outputs optimized for its own internal use — written for its own clinicians, structured around its own billing and compliance requirements, legible only within the context it was created in. A BCBA reads an ABA session note differently than a pediatrician does. A teacher can’t act on it at all.
So information accumulates inside systems while the people responsible for the same child operate without a shared picture of what’s happening.
A coordination layer doesn’t collect more data.
It makes existing data usable across the people responsible for the outcome.
Three things it actually has to do
The coordination layer is conceptually simple.
What makes it difficult is that no one has owned it.
Maintain a shared baseline
At a minimum, coordination requires a basic view of care beyond ABA:
- what services exist (speech, OT, school-based supports, medical care)
- who the key stakeholders are (pediatrician, diagnosing clinician, school, external therapists)
- where care is being delivered and at what level of intensity
In practice, this is rarely maintained in a consistent way.
ABA providers often don’t have a clear view of what else is happening with their clients — what the school is working on, whether speech goals align, or when the next diagnostic or medical interaction is scheduled.
Without that baseline, coordination isn’t difficult.
It’s impossible.
Translate — or show
Beyond the baseline, it has to translate information across contexts — or show it directly.
The detailed artifacts ABA providers already produce are valuable — but only inside ABA. Making them useful outside means converting them: extracting what’s active, what’s changed, what matters, and presenting it in a form that a teacher or pediatrician or caregiver can actually act on.
This is what makes a handoff usable. But translation has a fundamental limit.
Written summaries describe care. They compress it, filter it, and reframe it through the lens of whoever wrote them. By the time a session note becomes a caregiver summary becomes a pediatric update, significant meaning has been lost — not through negligence, but because language is lossy across disciplines.
Video changes this in a way written summaries can’t.
A short, structured clip of a communication attempt, a behavior being managed, or a skill being reinforced doesn’t require translation — it shows the thing itself.
A pediatrician can see behavior in context.
A teacher can observe how a skill is prompted.
A caregiver understands what consistency actually looks like at home.
Each person brings their own frame to it — and that’s the point. The shared reference does the work that written summaries can’t.
This is what makes video a coordination tool rather than just a documentation format.
Move the information
And finally, it has to move.
Coordination that doesn’t reach people isn’t coordination — it’s storage.
Whether that’s a translated summary or a short clip, the information has to flow through channels that already exist:
- patient portals
- caregiver communication tools
- whatever mechanisms providers may already use to stay in contact
The infrastructure is usually already there. The coordination function isn’t using it.
In some cases, coordination extends further. Not just sharing information—but shaping how care is delivered.
For example:
- aligning schedules across services to reduce conflicts
- providing scheduling support to external partners
(a diagnostician, a small speech provider, a school-based contact) - coordinating around key events like evaluations or plan changes
This doesn’t require controlling those services.
It reflects something else:
👉 one system taking responsibility for making the overall care experience function.
Most providers don’t do this. Not because it’s technically difficult—but because it expands the boundary of what they consider “their job.”
What it isn’t
A coordination layer isn’t a new platform. It doesn’t require replacing the systems that currently exist or forcing them into a shared model they weren’t built for.
It also isn’t system integration in the traditional sense — the attempt to get ABA platforms, EHRs, and school systems to exchange data directly. Those integrations have been tried. They work at the level of data transfer; they don’t solve the alignment problem. Data that crosses a boundary without being translated is still unusable on the other side.
And it isn’t a function that requires a new organization to own it. ABA providers already have the infrastructure — CRM systems, intake workflows, scheduling, communication tools.
Extending those systems to carry the coordination function is an operational choice, not a capital investment.
Where this approach runs into its own limits
There’s a boundary to what this model can do.
The coordination layer described here works within a relationship — between the ABA provider and the people around the client. It can make handoffs more usable. It can reduce the burden on parents. It can create a more consistent shared picture of care across a defined set of stakeholders.
What it can’t do is solve the structural problems that sit underneath all of this.
There is still no longitudinal patient model across systems.
There is still no shared definition of progress.
There is still no mechanism for cross-system decision support.
Some organizations have pushed further.
Providers like Cortica have built internal systems that:
- span multiple modalities
- maintain longitudinal views of care
- align clinical models across disciplines
Similarly, some Practice Management platforms are positioning to extend across service lines and potentially support broader coordination.
But these approaches share a constraint:
they work within a boundary.
- a single organization
- a defined platform
- a controlled set of services
Autism care extends beyond all of those.
So even when coordination works inside a boundary— it doesn’t carry across them.
These are not coordination problems. They are system-level problems.
Closing
Autism care doesn’t fail inside systems. It fails between them.
A coordination layer doesn’t fix the systems. It makes the space between them functional.
That’s not a small thing.
The parent who currently carries information from the ABA provider to the school to the pediatrician and back — that burden exists because the space between systems is unowned.
Owning it, even imperfectly, changes something real.
Today, that ownership is implicit — and usually external. This is about making it explicit — and internal.
The question for ABA operators isn’t whether coordination matters.
It’s whether they’re willing to own it—and operate differently because of it.